Chagas disease symptoms and treatment in humans

What Is Chagas disease?
Dr. Carlos Chagas discovered Chagas disease (pronunciation “CHAH-
Chagas disease is also called American trypanosomiasis and is related to African trypanosomiasis (The sleeping sickness caused by Trypanosoma
The blood-sucking bug Triatomine plays a significant role in the Chagas lifecycle. This bug is a meaner and larger cousin of the bed bug. The most common layman name reflects their tendency to bite especially in the face near the mouth: kissing bugs. Because they suck blood they are also called vampire bugs, and the bloodsucking is done with their cone-shaped nose, so they are also called
How common Is Chagas disease?
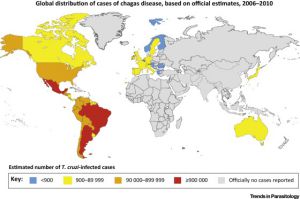
Chagas disease is mainly found in the southern part of the United States, in Mexico and in Mid- and South America. It is considered endemic in 21 countries (Citation: 5). Because of global migration patterns, the disease is spreading, especially to other parts of the United States and to Europe (Citations: 6, 7).
The world distribution of Chagas infections annually is shown here:
It is estimated that 8 million people are infected with T.
Is Chagas disease contagious?
When we think about the contagiousness of Chagas, we need to keep the life cycle in mind.
The disease is mostly transmitted through contact with feces of the Triatomine that contains the parasite Trypanosoma
There are other less common ways to get infected with
We don’t need to worry yet about common bed bugs giving us Chagas disease – although theoretically, this could be possible. (Citations: 11, 12).
What are signs and symptoms of Chagas Disease?
Chagas disease has two phases: the acute phase and the chronic phase. In both phases, the diseased can range from no symptoms to life-threatening.
Most people get no or only light self-limiting symptoms in the first weeks or months: like a rash and swelling at the site of the bite, swollen eyelids, fatigue or fever (Citation: 13). This acute phase can be severe in people with impaired immunity and (rarely) in young children, for example through infection of the heart or brain. Even if the symptoms resolve the infection will persist unless it is treated. An untreated infection will progress to the chronic phase, which is further discussed under complications.
How to diagnose Chagas Disease in humans?
Chagas disease is diagnosed through examination of your blood under the microscope. In the so-called “thick and thin smear” the laboratory staff will be looking for the T.
If you test positive you will often have to undergo cardiac examinations like X-ray and electrocardiogram and ultrasound, and if you have intestinal complaints often also an intestinal assessment.
If you wonder if you need to be tested for Chagas disease please see a healthcare provider.
What is the treatment for Chagas Disease?
For the treatment of Chagas disease, there are two pharmaceutical drugs available: benznidazole and nifurtimox. (Citations: 16, 17, 18). Both drugs are contra-indicated in early pregnancy (first trimester). The FDA has recently approved Benznidazole for use in children 2- 12 years old in the USA (Citation: 19), Nifurtimox is not FDA approved. Both drugs are available through CDC. (Citation: 20).
Treating Chagas disease takes an extended period of time. Benznidazole needs to be taken for 60 days, while Nifurtimox needs to be taken for 90 days. This treatment only cures the disease in the acute phase, in the chronic phase it might slow progression and complications. (Citation: 21)
What are complications from Chagas Disease in humans?
The main problems with Chagas Disease are deaths in young children (rare) and people with diminished immunity in the acute phase and the development of a chronic form of the disease. The chronic form can lead to heart problems (e.g. cardiac failure and even sudden death) and intestinal problems (enlargement of the esophagus and the colon – the lower portion of the large bowel). (Citations: 22, 23)
How to prevent getting infected with Chagas Disease?
Unfortunately, there is no vaccine yet against Chagas Disease. Several therapeutic and preventive vaccines are in development (Citations: 24, 25). Prevention takes into account the various ways of transmission and the life cycle (Citation: 26):
- Preventing bites through use of protective clothing, insect repellents that contain DEET for exposed skin and sleeping under an insecticide-treated mosquito net.
- Preventing the entry of the kissing bugs into your house through home improvements (plastering walls, concrete floors, corrugated iron roofs) and insecticide spraying of house and surrounding
- Making sure bug feces can’t get into your food and drinks: safe handling and storage of food including good hand hygiene
- Only using safe blood (for transfusions) and safe organs (for transplantation) through screening of donors for T.
cruzi . - Safety protocols in laboratories to prevent contact with infected materials
WHO plays a key role in global control of Chagas disease (Citation: 27)
References
- The discovery of Chagas disease (1908-1909): great successes and certain misunderstandings and challenges José Rodrigues Coura https://www.scielo.br/scielo.php?script=sci_arttext&pid=S0037-86822013000400389 (Retrieved: 9/9/2017)
- WHO Fact sheet: Chagas disease (American trypanosomiasis) https://www.who.int/mediacentre/factsheets/fs340/en/ (Retrieved: 9/9/2017)
- Trypanosomiasis, human African (sleeping sickness) https://www.who.int/mediacentre/factsheets/fs259/en/ (Retrieved: 9/9/2017)
- Bloodsucking Conenose Found: Don’t Panic! http://bygl.osu.edu/index.php/node/426 Authors: Joe Boggs, Cindy Meyer Published on July 13, 2016
- Pan American Health Organization (PAHO) General Information – Chagas Disease https://www.paho.org/hq/index.php?option=com_content&view=article&id=5856&Itemid=41506&lang=en
- Trypanosoma cruzi and Chagas’ Disease in the United States https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3194829/
- Epidemiology of Chagas disease in Europe: many calculations, little knowledge. https://www.ncbi.nlm.nih.gov/pubmed/23989652
- https://www.who.int/chagas/epidemiology/en/
- https://www.paho.org/hq/index.php?option=com_topics&view=article&id=10&Itemid=40743
- https://www.cdc.gov/parasites/chagas/epi.html
- Bed Bugs And Chagas Disease: Don’t Worry Quite Yet https://www.popsci.com/bed-bugs-and-chagas-disease-dont-worry-quite-yet
- Bed Bugs (Cimex lectularius) as Vectors of Trypanosoma cruzi https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4347337/
- https://www.cdc.gov/parasites/chagas/gen_info/detailed.html
- https://www.cdc.gov/parasites/chagas/diagnosis.html
- https://www.who.int/chagas/disease/home_diagnosis_more/en/
- https://apps.who.int/medicinedocs/en/d/Jh2922e/2.11.1.html#Jh2922e.2.11.1
- https://apps.who.int/medicinedocs/en/d/Jh2922e/2.11.2.html
- https://www.mayoclinic.org/diseases-conditions/chagas-disease/diagnosis-treatment/treatment/txc-20322137
- https://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm573942.htm
- https://www.cdc.gov/parasites/chagas/health_professionals/tx.html
- https://www.mayoclinic.org/diseases-conditions/chagas-disease/diagnosis-treatment/treatment/txc-20322137
- https://www.mayoclinic.org/diseases-conditions/chagas-disease/symptoms-causes/dxc-20322128
- https://www.cdc.gov/parasites/chagas/treatment.html
- https://www.nature.com/articles/s41541-017-0010-z
- https://www.ncbi.nlm.nih.gov/pubmed/27737611
- https://www.who.int/chagas/disease/prevention/en/
- https://www.who.int/chagas/strategy/overview/en/
Watch Videos To Learn More