Hookworm and Cutaneous larva migrans symptoms and treatment in humans
What Is a Hookworm infection?
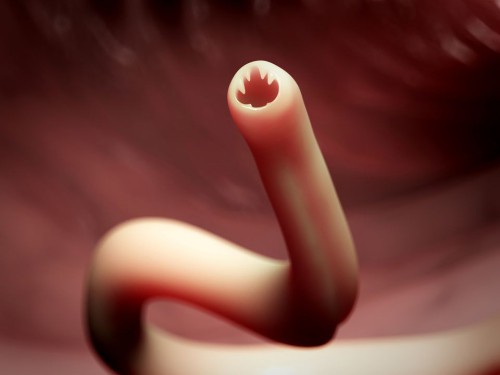
Hookworm is an intestinal parasitic roundworm (or nematode) that can infect humans and animals. (Citation 1) The name comes from the “hooks” at the worm’s mouth that helps it to attach to the host’s intestines. Hookworms can infect the human intestines – this is typically called a hookworm infection. It can also infect the human skin, and when it infects the skin it is called cutaneous larva migrans (creeping eruption or sandworm disease).
The main intestinal hookworms in humans are Ancylostoma duodenale and Necator americanus. (Citation: 2, 9)
Creeping eruption is typically caused by Ancylostoma species, especially the dog or cat hookworm Ancylostoma braziliense. (Citation: 3, 9)
How common are Hookworm infections?
According to estimates, there were 438.9 million people infected with hookworm worldwide in 2010, especially in developing countries. (Citation: 4) Hookworm infection was common in the past in Europe and the USA. The level of infections declined over a few decades but is now on the rise again. Some attribute the increased rate of infection as being imported by travelers or migrants from developing countries. As people stopped receiving treating for these infections, it allowed the infections to spread without hindrance. Children are especially at risk of hookworm and creeping eruption because of playing and going around barefoot. Cutaneous larva migrans is found worldwide, but more often in tropical areas. (Citation: 5)
Are Hookworm infections contagious?
To understand how the hookworm infections spread, it is important to understand their lifecycle. The CDC has made a nice graphic display. (Citation: 5)
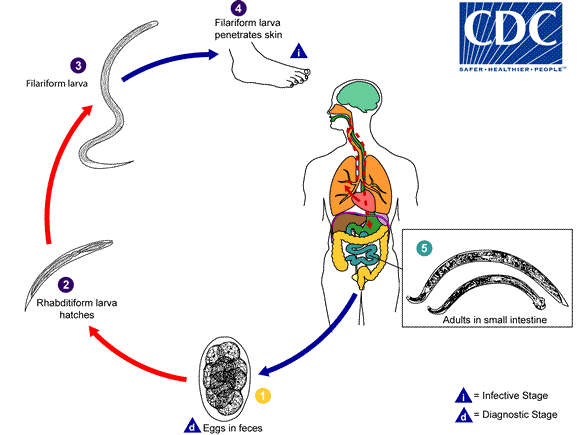
Once eggs are passed in the stool, they require a gestation period to grow. Ideally, it would be a warm, moist, shaded sand or soil. It takes about one or two days to turn into a larva. After 5 to 10 days they can infect other humans and animals: they directly penetrate through the skin. The blood carries the larvae to heart and the lungs. Once the larvae pass through the lungs, they go up the pharynx and then are swallowed and move to the small intestine where they use their hooks to attach to the wall and suck blood. They can easily remain for 1-2 years but might stay for longer without treatment.
The key role of soil for the transmission of helminths (parasitic worms) like hookworm, is characterized by the internationally recognized term “soil-transmitted helminths”. (Citation: 6) The soil assists with the transmission of the infection indirectly from the person (or animal) to the person (or animal), there is no direct person-to-person transmission.
Creeping eruption is caused by larvae that develop from the hookworm eggs in cat and dog feces. These eggs develop properly if the feces is located in warm or moist soil and sand. When someone walks, sits or lies down unprotected on this soil or sand, then the larvae penetrate the skin.
Signs and symptoms of a Hookworm infection
Hookworm infections are often without (obvious) symptoms. When the hookworm larvae enter the skin, there might be an itchy rash. The migration of the larvae through the lungs sometimes results in the Löffler syndrome (see description below under complications). Adult worms can initially cause upper abdominal pain, loss of appetite and weight loss, diarrhea and gas formation. A chronic and/or heavy infection (many worms) leads to iron deficiency anemia and protein loss. (Citation: 1)
Creeping eruption is often seen in areas that are likely to come into contact with infected soil or sand: feet, legs, back or buttocks. (Citation: 2) When the larvae (immature worms) enter the skin there might be a burning or tingling sensation. The larvae might start creeping immediately after entry or be quiet for weeks to months. Once they start creeping there will be intense itching and the formation of 2-3 mm wide snake-like tracks which advance a few millimeters to centimeters per day. (Citation: 5)
How to diagnosis Hookworm infections in humans?
Hookworm infections are usually diagnosed by finding the hookworm eggs under the microscope in the (concentrated) stool of the infected human or animal. (Citation: 7)
Creeping eruption is usually diagnosed by the history and the outlook of the skin. In rare cases, especially if other methods have to be excluded, a skin biopsy or blood test for serology or eosinophilia is needed. (Citation: 8)
What is the treatment for Hookworm infections?
Treatment for hookworm infection includes dosing orally with Albendazole (single dose), Mebendazole (3 days or single dose) or Pyrantel pamoate (3 days). (Citation: 1)
Treatment for cutaneous larva migrans is either topical with thiabendazole cream for 5 days or orally with albendazole (3 to 7 days) or ivermectin (1 to 2 days). Topical treatment is used for small localized lesions (1 or few larvae), while oral is used for more widespread lesions (more larvae) or if the topical treatment did not work. (Citation: 5)
Are there complications from Hookworm infections?
Complications of hookworm infection are mostly iron deficiency anemia and protein loss – both due to blood loss from the sucking hookworms. If the infection is heavy and/or long-lasting the iron and protein loss will lead to stunted growth and mental development in children. (Citation: 10)
Complications of creeping eruption include secondary bacterial infection of the skin lesions (Citation: 11) and the Löffler syndrome. The Löffler syndrome is a response by the lungs and blood to the parasite infection. The symptoms are mostly dry cough, sudden changes in the chest X-ray and increase of eosinophils in the blood. This syndrome usually disappears within one month. Symptomatic treatment with corticosteroids might be used. (Citation: 12)
How to prevent Hookworm infections?
The primary preventive measure for both hookworm infection and cutaneous larva migrans is avoiding contact with soil or sand that is contaminated with (animal and/or human) feces. This can be done through safely disposing of feces and not going barefoot or sitting unprotected on the soil. Because these measures are often difficult to implement, regular mass drug treatment of susceptible groups called MDA (mass drug application) with albendazole or mebendazole – add (WHO factsheet ref ) is used in high-risk areas. (Citation 5, 13) Pets (cats, dogs) should also be treated for hookworm, especially to prevent cutaneous larva migrans. (Citation: 1)
References
References:
- Centers for Disease Control and Prevention. Accessed online 15th September 2017. Weblink: https://www.cdc.gov/parasites/hookworm/gen_info/faqs.html
- Merck Manual Professional Version. Accessed online 14th September 2017. Weblink: http://www.merckmanuals.com/professional/infectious-diseases/nematodes-roundworms/hookworm-infection
- Merck Manual Professional Version. Accessed online 14th September 2017. Weblink: http://www.merckmanuals.com/professional/dermatologic-disorders/parasitic-skin-infections/cutaneous-larva-migrans
- Pullan and others in “Global numbers of infection and disease burden of soil transmitted helminth infections in 2010” in Parasites & Vectors. 2014; 7:37. Weblink: https://parasitesandvectors.biomedcentral.com/articles/10.1186/1756-3305-7-37
- Centers for Disease Control and Prevention. Accessed online 15th September 2017. Weblink: https://www.cdc.gov/parasites/hookworm/biology.html
- World Health Organization. Accessed online 15th September 2017. Weblink: http://www.who.int/gho/neglected_diseases/soil_transmitted_helminthiases/en/
- Centers for Disease Control and Prevention. Accessed online 15th September 2017. Weblink: https://www.cdc.gov/parasites/hookworm/diagnosis.html
- New York Times - Health. Accessed online 15th September 2017. Weblink: http://www.nytimes.com/health/guides/disease/creeping-eruption/overview.html
- Accessed online 15th September 2017. Weblink: https://medlineplus.gov/ency/article/000629.htm
- Centers for Disease Control and Prevention. Accessed online 15th September 2017. Weblink: https://www.cdc.gov/parasites/hookworm/disease.html
- DermNet New Zealand. Accessed online 15th September 2017. Weblink: https://www.dermnetnz.org/topics/cutaneous-larva-migrans/
- Merck Manual Professional Version. Accessed online 15th September 2017. Weblink: http://www.merckmanuals.com/professional/pulmonary-disorders/interstitial-lung-diseases/l%C3%B6ffler-syndrome
- World Health Organization. Factsheet on Soil-Transmitted Helminths. Accessed online 15th September 2017. Weblink: http://www.who.int/mediacentre/factsheets/fs366/en/
Watch Videos To Learn More

